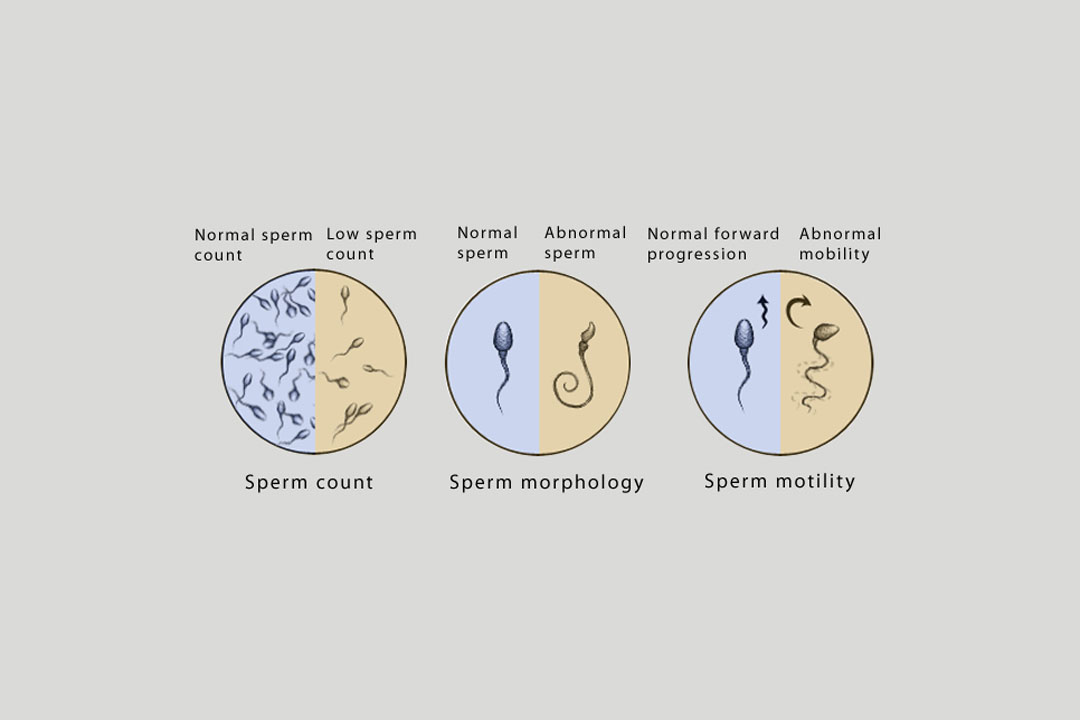
In roughly 40% of infertility cases, male factor infertility plays a role. We begin testing with a sperm analysis. Consulting with a reproductive endocrinologist and urologist is helpful in evaluating infertility factors and can suggest various fertility treatment measures that can preserve your potential for having children in the future, including sperm sample preservation.
In some cases, the type of fertility intervention can be modified to work best with any female fertility factors. Treatment for male factor infertility is extremely successful, even with very few sperm, ejaculated or surgically retrieved.
Mild Male Factor: In those with more than 10 million motile sperm, fertility can be enhanced with sperm preparation and insemination of prepared sperm into the uterus, or IUI.
Moderate to Severe Male Factor: In patients with less than 10 million motile sperm, IVF yields more successful pregnancy rates. If complex abnormalities exist in the number, motility, or shape, intracytoplasmic sperm injection (ICSI) produces higher fertilization rates.
Those with severe male factor infertility may carry genetic factors that should be investigated prior to fertility treatment. Severe factors include chromosomal abnormalities (Klinefelter syndrome, abnormalities in the Y chromosome), and abnormalities in cystic fibrosis genes (bilateral absence of the vas deferens). We will thoroughly investigate these factors during the initial workup to determine the best course of action in your fertility care.
Types Of Male Factor
Azoospermia: No sperm appear in the ejaculate due to obstruction in male ducts or markedly reduced sperm production:
Obstructive Azoospermia: Obstruction can be genetic (congenital bilateral absence of vas deferens) or acquired (after vasectomy). Treatment options include sperm retrieval to be used in IVF or surgical removal of obstruction. In general, surgical sperm retrieval and IVF tends to be more successful, but if the patient decides to undergo surgery to relieve obstruction, it is important to retrieve sperm for preservation in case surgery is unsuccessful.
Non-Obstructive Azoospermia: Decreased sperm production could also be genetic (Kleinfelter syndrome, Kallmann syndrome, abnormalities in Y chromosome) or acquired (following chemotherapy). In this case, we first search for sperm in semen samples, if none found, sperm can be directly retrieved from using an outpatient surgery (TESE).
Erectile Dysfunction: Men with difficulty maintaining erection or ejaculation can be assisted by noninvasive methods of obtaining sperm that can be frozen or used immediately to achieve pregnancy.
Retrograde Ejaculation: In some men, sperm may flow backwards into the urinary bladder. Sperm can be retrieved from a urine sample or directly from the testes.
Vasectomy: This is an example of obstructive azoospermia. Men with prior vasectomy and want to father children can undergo vasectomy reversal.
Alternative options to vasectomy reversal:
- Use previously frozen sperm
- Harvest sperm from the testes and use in IVF while leaving the vasectomy in place for long term contraception.
The choice of treatment should include evaluation of female factors. Also even if vasectomy reversal is contemplated, sperm should be obtained during the reversal and frozen in case reversal is not successful.
Varicocele: These are dilated veins around the testes. Although some varicoceles are associated with abnormal sperm parameters, there is no strong evidence that varicocele repair increases the odds for pregnancy in female partners.
Call NYC IVF to schedule an appointment and diagnose the factors affecting your fertility. Call (800) 853-7595 to schedule a consultation!