Fertility Treatments
At New York City IVF we strive to apply the simplest possible fertility solution that yields a reasonable pregnancy rate first. It gives us and our patient’s great satisfaction to be able to help them conceive with the aid of minimal intervention rather than advanced technology whenever possible. It is our philosophy of care to try simple methods first.
Simple Fertility Treatments
Timed Intercourse
Preconception counseling should be strongly considered before attempting to conceive to uncover any preventable medical or genetic issues.
Timing of sexual intercourse for the majority of couples should be the initial step towards conception. Having intercourse three times per week maximizes the chance for natural conception without monitoring of ovulation.
Ovulation can be monitored using the commercially available ovulation prediction kits, which are more accurate than assessing cervical mucus or measuring basal temperature. When the kit indicates a surge, ovulation usually ensues 1-2 days later. Ultrasound can also be used to confirm development of follicle. Intercourse should be started the next day after a surge for 3 successive days.
Lifestyle modification includes avoiding smoking and excessive coffee intake. Women should also take one pill of prenatal vitamin per day that contains one mg of folic acid.
The chance for spontaneous conception is decreased with increased female age and long duration of unprotected intercourse.
The chance for spontaneous conception starts to drop at age 30.
Probability of getting pregnant is 20% per cycle in the first 6 months, 15 to 10% in the second 6 months. A total of 80% will conceive by the end of the first year. The odds continue to drop to 3-5% per month towards the end of the second year (another 10% will conceive) and 1% per month in the third year (less than 5% will become pregnant in the third year of trying).
Ovarian Stimulation And IUI
In many situations mild stimulation of the ovary (or even without stimulation) followed by intrauterine insemination (IUI) is a simple and friendly fertility treatment. This could be a reasonable treatment for women with mild male factor, ovulatory disorder or unexplained infertility.
It entails
- Administration of oral medication (clomid or aromatase inhibitor) or injections (gonadotropins)
- Monitoring of follicle development with ultrasound and estrogen levels. This is the most critical step. Careful monitoring and dose adjustment is required to avoid multiple follicle development which increases the risk for multiple pregnancies.
- Triggering ovulation (using an injection)
- Sperm preparation (by washing and concentrating sperm) and injecting the prepped sperm through the cervix followed by bed rest for a few minutes.
The pregnancy rate after this procedure is about 10 to 15% per each cycle of treatment. It is reasonable to try this simple intervention for two to three cycles before proceeding to more advanced methods.
Following ovarian stimulation and intrauterine insemination (IUI) multiple pregnancy can occur if more than one follicle is produced. The incidence of twins after clomid stimulation is about 8% and after FSH stimulation is 30%. Higher order pregnancies (triplets or more) is 1% after clomid stimulation and about 3% after FSH stimulation. The number of embryos reaching the uterus after triggering ovulation cannot be controlled.
When Ovarian Stimulation And IUI Should Be Avoided
For women at risk for robust response to fertility medications especially injections (resulting in the development of multiple eggs) the question becomes should she proceed with this option or abandon it in favor of IVF where the number of embryos transferred to the uterus can be controlled? When IVF is performed, the number of embryos transferred into the uterus is under the control of the patient and the physician. A single embryo can be transferred, avoiding multiple pregnancy and its long term risks to the babies. Extra embryos are frozen.
If ovarian stimulation is selected, fetal reduction should be discussed in detail.
Advanced Fertility Treatments
Why NYCIVF Is For Advanced Fertility Treatments
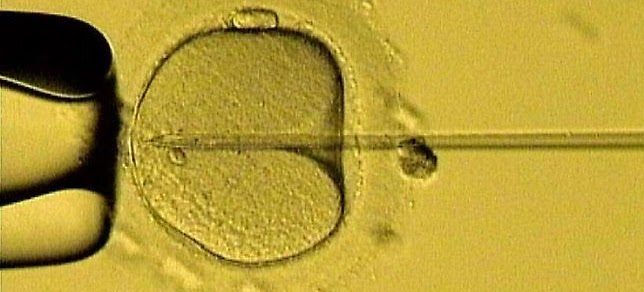
In some women and men advanced fertility treatments are the better approach. They carry a higher chance for success and a safer way to achieve pregnancy. Assisted reproductive technologies also provide reproductive options for men and women not available with simple fertility treatment.
These include women with blocked fallopian tubes, severe male factor infertility, repeated unsuccessful IUI, diminished ovarian reserve, when parents carry a genetic abnormality, in women at high risk for multiple pregnancy e.g. PCOS and professional women who want to freeze their eggs for future reproduction. It is also used for fertility preservation in women diagnosed with cancer and when gestational carriers are needed.
Advanced fertility treatment requires retrieval of eggs, assisted fertilization and culture of embryos in the laboratory. Embryos can be genetically tested and can be frozen for later use.
